 In my pharmacy resident days, I spent a lot of time counseling patients about their medications. A good majority of this work included documenting a complete and accurate medication profile. Seems pretty simple, right? Not so much.
In my pharmacy resident days, I spent a lot of time counseling patients about their medications. A good majority of this work included documenting a complete and accurate medication profile. Seems pretty simple, right? Not so much.
Many patients may have multiple conditions that require them to see multiple providers. They may even get their prescriptions dispensed at more than one pharmacy. We usually saw them during their hospital stay or clinic visit where they likely did not bring all their home medications with them. Many patients didn’t even know the name and dosage (or even the reason) for the medications they were taking. We had to call pharmacies and providers to track down all the necessary information. Sometimes we could get historical information from the chart – electronic health records definitely made that easier – and sometimes we couldn’t. When trying to get this information from other providers, we often ran into issues requiring multiple requests, and we still didn’t receive the information right away.
Then Congress passed the 21st Century Cures Act in 2016. One provision in the Cures Act addressed information blocking and required the Office of the National Coordinator of Health IT (ONC) and CMS to define and enforce rules governing the sharing of health data. Earlier this year, ONC released its final rule on information blocking, which outlines in detail how health systems, health information exchanges (HIEs), and health IT developers can meet these requirements.
The requirements are phased, but parts of the rule go into effect as early as Nov. 2, 2020. The first requirements mandate releasing a defined set of data, specifically United States Core Data for Interoperability (USCDI v1), and responding to requests within 10 days. As organizations continue to face challenges caused by COVID-19, it may be difficult to meet these requirements in such a short timeframe when resources are already stretched thin.
If you’re wondering how these changes may impact your organization, here are five areas to consider as you begin planning for the upcoming deadline.
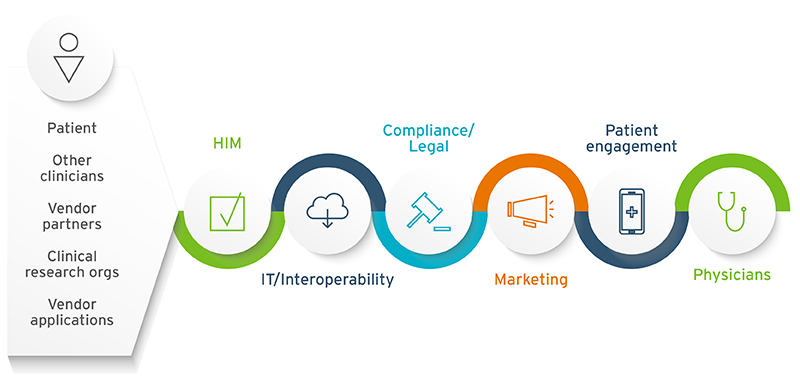
Start with IT but don't end there
You may think ensuring your EHR captures all the data needed for this first phase of information blocking requirements is all you need to do. That work will definitely need to be done, but first, you’ll need to complete validation with operational stakeholders to review methods and processes for sharing data. Meeting the requirements of this rule means examining processes and workflows in many areas of the organization.
HIM
Gone are the days when a patient may have gone down to the medical records office in the basement and a huge file or CD was produced. While that may still be necessary for some types of data, the bigger question now is how will variable requests for data be fulfilled? There will likely be an increase in volume of requests, and you will have to track and document responses to requests within a 10-day period. You will also need to examine and potentially change current processes to accommodate the new requirements.
Compliance/legal
The final rule is a short 200-page document. You will definitely want your compliance and legal departments to review the rule and weigh in on any needed policy and procedure changes. You also want to take into account state and HIPAA regulations because they may be more stringent than the information blocking rules.
Patient happiness
The patient is at the center of the Cures Act. Whether you have a marketing department, an area focused on patient engagement, or both, you will want to make sure you examine how your patients currently receive their health information and communicate what changes they can expect. There will likely be new processes for requesting that information and new methods or apps that will be available for them to visualize their data. Also, they will probably see more information than they did before, which will likely generate questions.
Physician satisfaction
You may be thinking, "What does this have to do with doctors?" As mentioned above, patients may receive more information than they have in the past, and this could generate questions and concerns. The doctor's office will likely be one of the first places the patient will call if and when they see something that sparks a question.
Although the data that must be shared in November is limited to USCDI v1, it does include clinical notes and lab results. In the past, these were not required or could’ve been delayed until the physician could communicate potentially sensitive information to the patient. Physicians may also be concerned that their previously confidential notes are now open for patients to see. Organizations will need a solid communication plan and education in place for providers to understand and effectively meet the requirements.
To be ready for these requirements by November, leaders will need to identify and bring together the many stakeholders that this affects within their organization. The team will need to conduct a gap analysis, and coordinate the various and interconnected tasks that will be needed. Health systems must keep in mind this is the first step in a larger effort to give patients access to all of their health information electronically by 2022. Oh, and not to mention, help those pharmacy residents of tomorrow.
If you’d like to learn more about the impending information blocking rules, please join our webinar on Aug. 11 from 11 a.m.–noon Central. I’ll be there along with my Nordic colleagues to discuss the implications of these rules and how your organization can prepare.





